People could be forgiven for initially believing that COVID19 is just like the flu, as many have personal experience with the flu and gotten used to the risk posed by the flu.
This tendency towards complacency was reinforced by bad takes in the media or from academia along the lines of “the real risk is hysteria”.
To be fair: Panicking is rarely helpful and it is important to put potential risks into perspective.
The flu is indeed serious, but we have a good idea of just how serious it is likely to be. This is due to the fact that it is happening every year and that we have been observing the seasonal flu for a long time, so there is plenty of data.
Here, we graphed the annual mortality attributed to the flu in the United States for the past 40 years, as reported by the CDC. We have data going beyond that time period, but it is hard to integrate, as reporting criteria have changed, and it is not easy to estimate how many people actually die from the flu, as a large proportion die from secondary pneumonia, not influenza per se. So for an apples to apples comparison, we keep it at this.
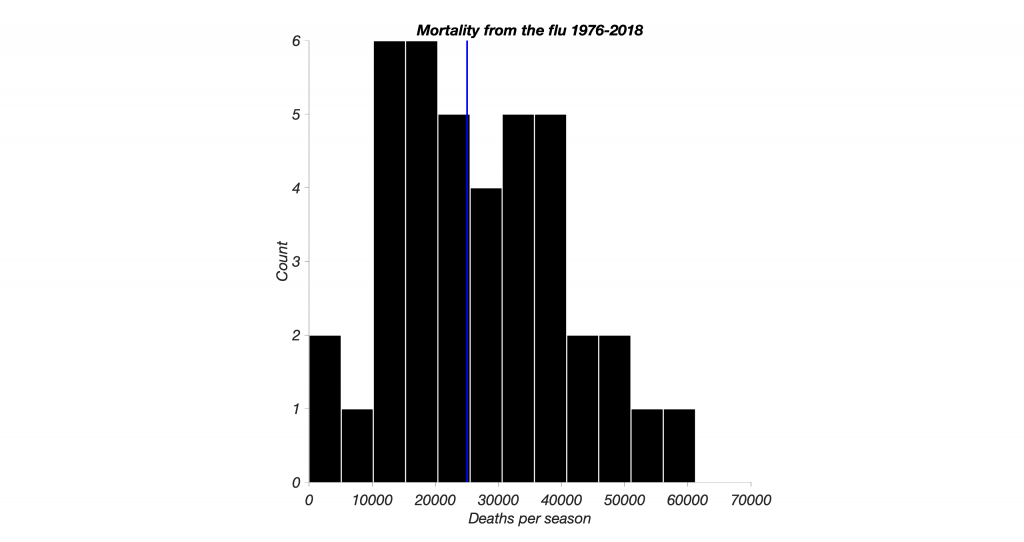
This graph is a frequency histogram. Black bars represent how often a flu season led to a given number of deaths. For instance, twice in the past 40 years, flu claimed less than 5000 people a year (the left-most bar). As you can see, the distribution of mortality due to the seasonal flu is roughly normal – albeit with a slight skew. The expected death rate from a given seasonal flu is captured by the blue line, which represents the median, at about 25,000 cases. Importantly, how deadly any flu season can be expected to be clusters in a narrow range around this central value. There was only a single flu season in the last 40 years with more than 60k deaths, in 2017/18. A few times, the flu season was mild, such as in 1986/7 and 1978/9, with 3,349 and 4,681 cases, respectively.
In other words, we more or less know what to expect from the seasonal flu – the range of typical outcomes is rather narrow within about one order of magnitude, and while 25k cases is a serious toll for the United States as a whole (about 2/3 as many as people who die in car accidents per year), the individual annual risk is low, at around 1 in 14,000.
The coronavirus – which leads to COVID19 is not like that, because it is new, so we do not know how the mortality from COVID19 distributes, yet. Early reports indicate that it is highly contagious (every person who has it seems to infect 2.5 others, compared with about 1.3 for the seasonal flu) and mortality seems to be high, with between a 2% and 3% of the people who test positive die from the disease, on average.
The very fact that these numbers are very much in doubt – mortality estimates in the literature vary widely, depending on how many cases are tested – reflects how much uncertainty there is about COVID19, at this point.
Let’s assume that people treat it just like the common flu and don’t implement serious social distancing or containment measures. In that case, we can expect that 50% of the US population will eventually get this virus and 1% will die from it (these estimates are extremely conservative, as experts believe that up to 80% of the population could get infected in this case, and that the mortality could be up to 3.5%).
In that case, we could expect close to 2 million fatalities from COVID19 in the United States alone. This sounds dramatic, but is in line with the outcome of the last severe pandemic. To put this in the context of the seasonal flu, we now represent this estimate in the same graph as above, as a red line.
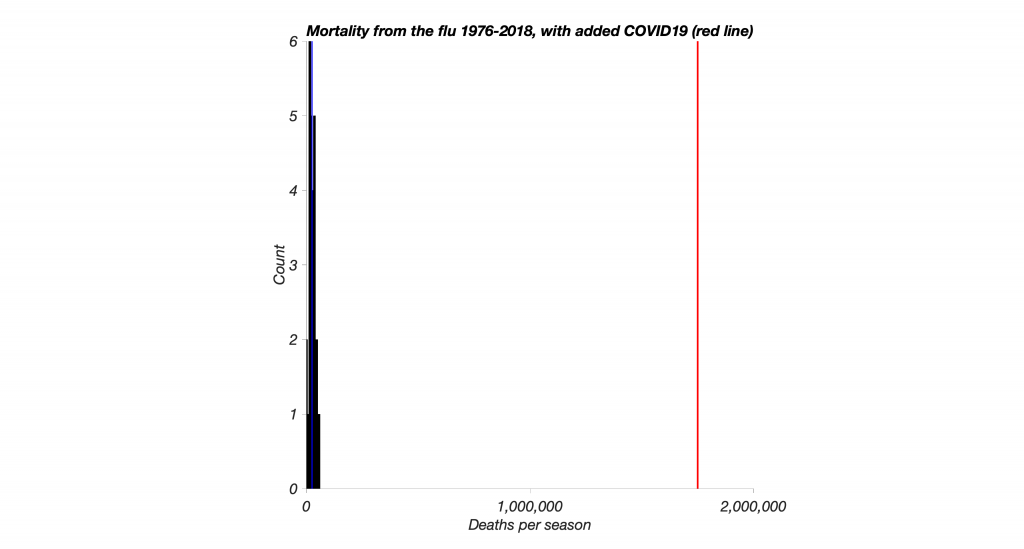
If the experience in Wuhan and Italy is any indication, the reason for this terrible death toll is mostly due to a local lack of ventilators, which leads a serious case of the illness to take a fatal turn.
The good news? It appears that this terrible outcome is entirely preventable. Containment (as in China), massive testing (as in South Korea) and early intervention (as in Taiwan and Singapore) seem to have curbed the devolvement of the situation into a million+ fatality scenario in each of these countries. It’s not entirely clear what the role of factors like temperature (particularly in Singapore) is, but it is highly encouraging that we can prevent a catastrophic outcome if we do take the disease seriously enough, early enough.
So let’s assume that we take decisive action (social distancing, hand washing – with soap, no face touching, lots of testing) and we get the same outcome as China, which is actually a pessimistic take, as our population is much smaller. That outcome is now represented in green – it would manifest as a bad flu. In other words, if we take such actions now, cases will likely mount for another month or so, but then peter out by mid-April.
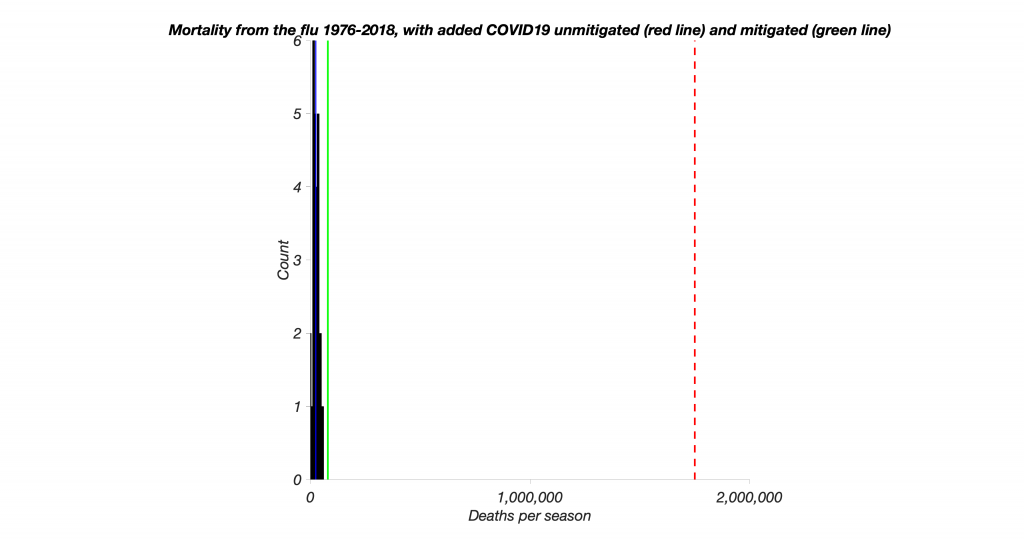
Of course, reality is highly ironic. If there are no good options available, leaders will not get credit for taking the bad option that prevents a catastrophic outcome, as the counterfactual is not observable. Thus, it is particularly important to keep that in mind and act – decisively – as soon as possible.
Action potential: The virus has the potential to be catastrophic, but doesn’t have to be, if people do the right thing now.
thank you pascal. best article i’ve read on this yet. thank you for being so rational
I think we all have to take the virus really serious